Technical Specialties

Electronic Medical Records
Our experts have deep front-end and back-end experience building clinician documentation workflows and configuring aspects for how information is stored and retrieved across many major EMR vendors

Audit Trails
Certified electronic medical record systems provide tamper-resistant tools to enable a skilled forensic expert to audit patient records and system logs to produce a complete history or all access, documentation entries, medication and provider orders and clinical decision support (CDS) patient safety alerts
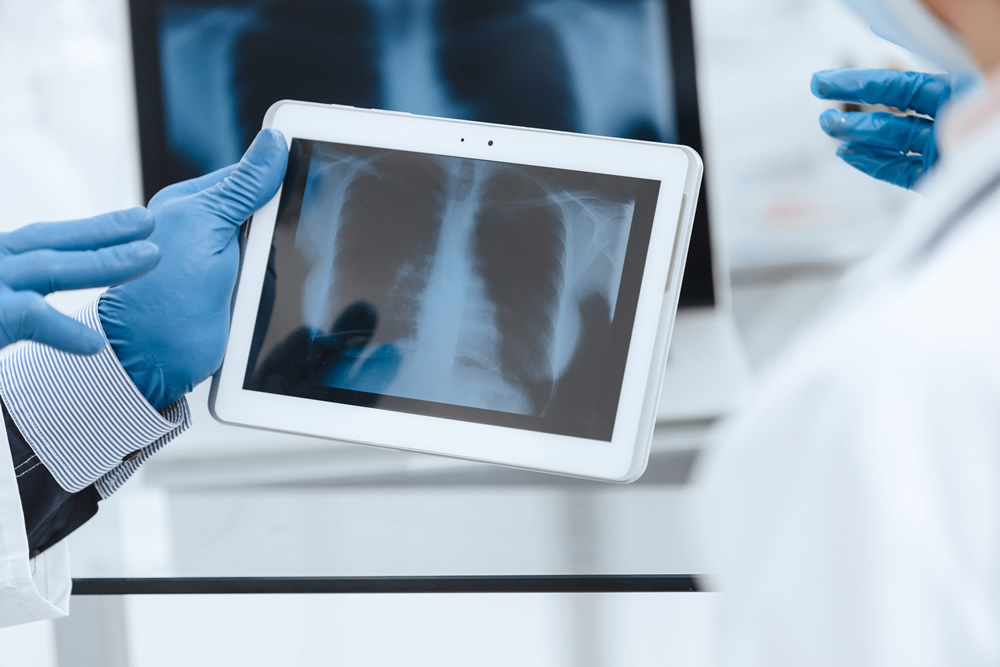
Digital Forensics
Our team of data analysts and clinical informaticists can examine and analyze large volumes of structured data to discover patterns of policy noncompliance or fraudulent behaviors

Data Retrieval
Our business intelligence experts understand the the intricacies of healthcare databases and can write queries to extract valuable metadata beyond what is provided in typical legal medical record documents
- In-depth knowledge of popular electronic medical record software
- Knowledge of investigative methods to locate specific electronic data (navigating records with analyst profile credentials)
- Designing and building custom processes to facilitate evidence collection (SQL queries)
Clinical Specialties

Clinical Informatics
Our board certified clinical informatics specialists have years of experience with implementation, optimization, maintenance and reporting measures of electronic medical records and clinical applications and served in leadership, strategic, change management and financial planning roles within health systems and IT consultancy

Nursing Specialties
Our team of nurse experts can provide expert clinical insights and technology utilization from the bedside across practices settings and specialties such as adult and pediatric intensive care, emergency, surgery, case management and more
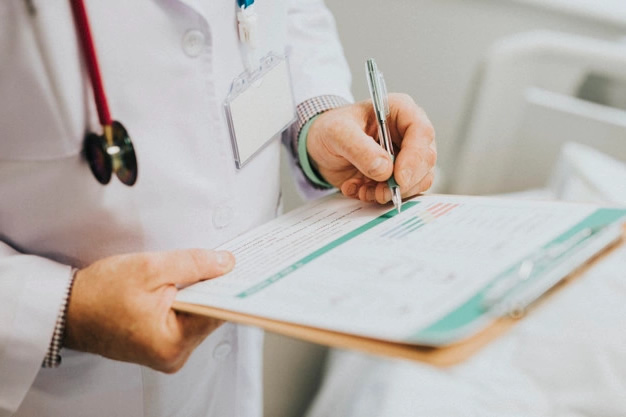
Documentation Workflows
The pressure of providing high quality care in complex, time-sensitive environments often leads to providers taking shortcuts or inventing workarounds when it comes to patient chart documentation. Our team can evaluate user education to determine whether your case involves provider negligence.

Policies & Procedures
Hospitals and provider offices establish written guidelines for use of healthcare IT systems by their staff to govern expected behaviors, which can provide case insights or identify negligent perpetrators
Common Case Examples
Missed or Delayed Diagnosis
A failure to recognize clinical symptoms and signs, review pertinent lab results, order relevant tests or research and act on additional information, or have the patient referred can make a big impact on a person’s life and are all events and actions that are readily traceable within the healthcare professional’s EHR system.
Failure to Treat
The failure to treat a patient adequately can show up when a patient is released too soon from a facility or hospital, not provided with instructions for caring for a condition or follow-ups, not ordering relevant medical exams or tests, not considering a patient’s medical history, or having too large of a patient base to adequately take care of each patient. Clues to piecing this picture together can be found across interdisciplinary documentation workflows and help recreate an accurate timeline of events.
Surgical or Procedural Errors
Common surgery mistakes include surgery being done on the wrong body part or patient; problems with anesthesia; failure to follow accepted practices before, during, and after the procedure; not communicating vital information to avoid an error; and/or leaving devices, tools, or other materials in the patient that should never be left permanently. The EHR serves as almost a silent observer to these situations collecting data from devices, monitoring systems as well as direct input from a variety of clinicians and provides key metadata that can demonstrate precisely what went wrong and when.
Prescription Drug or Medication Administration errors
- From severe allergic reactions to loss of life, medication errors that occur from prescribing, filling or administering drugs can have fatal consequences. Errors can include prescribing the wrong type of medicine, the incorrect dosage, not recognizing a dangerous drug interaction or allergic reaction, or failing to recognize the signs of addiction or abuse for at-risk patients. EHRs vendors have designed decision support safeguards and tools to help providers avoid making these kinds of mistakes, and a provider’s interaction with these alerts are recorded in accordance with federal requirements.
- Additionally, clinicians that administer high-risk medications may inflict serious harm if established safety guidelines or practices are not properly followed. The entire lifecycle of a medication administration is meticulously recorded in EHRs allowing for very detailed timelines to be created and identify all parties involved from the moment a drug order is entered by a provider through the time of entry into the patient’s body in many cases.
Childbirth Injuries
Birth injuries can happen at any time during pregnancy, labor or delivery with childbirth being an exceptionally critical time both for the mother and infant. Examples of substandard care include not receiving a notice of any prenatal health conditions before birth; failure to perform a C-section when the circumstances necessitate it; not recognizing fetal distress; improperly using forceps or excessive force to separate the baby from the birth canal; not taking care of the umbilical cord around the baby’s nose, mouth, or neck; and/or mishandling the baby. The resulting effects of these care deviations include cerebral palsy, bone fractures, spinal cord injuries, hypoxic-ischemic encephalopathy (HIE) and postpartum hemorrhage, which is the leading cause of maternal death after delivery. In today’s labor & delivery units, medical devices are constantly monitoring both the mother and baby and communicating with the local EHR system, exchanging critical information about the entire delivery process from start to finish.
Bedsores
Bedsores (also known as pressure ulcers or pressure injuries) form when a patient with debilitation or reduced mobility is left in the same position for too long. Bedsores are a sign of neglect or inadequate care commonly seen in hospitals and nursing homes, and if left untreated, bedsores can become infected and lead to longer hospitalizations and more serious health problems. Healthcare facilities have strict policies in place for proper procedures to prevent these unnecessary situations from occurring and prescribe specific documentation guidelines for accurately tracking the efforts within the EHR system.
Hospital Infections
While hospitals and medical staff are equipped to handle any emergency, they also can transmit harmful pathogens to patients within their care, resulting in hospital-acquired infections (HAIs). In order to qualify, the infection must occur up to 48 hours after an admission, up to 3 days after discharge or up to 30 days after a surgery, any of which must be in a medical facility which the patient was admitted to for reasons other than the infection. Common types of HAIs include central line-associated bloodstream infections (CLABSI), catheter-associated urinary tract infections (CAUTI), surgical site infections (SSI), and ventilator-associated pneumonias (VAP). Infection prevention teams use the EHR system to surveil the entire population of admitted patients by targeting data that can be used to pinpoint all of the qualifications and timelines throughout any patient’s hospitalization and any subsequent office visits or readmissions.











